Tobacco use was defined as current tobacco use. The main independent variables of interest were age, sex, tobacco use, history of previous surgical intervention in the same ear, history of tympanostomy tube placement, and surgical technique. The outpatient clinic visits included the total number of regularly scheduled visits and patient-initiated visits for any mastoid bowl health concerns.

The number of postoperative outpatient clinic visits per 6-month interval up to 4 years was collected (i.e., number of visits for 0–6 months, 6–12 months, 12–18 months, 18–24 months, 24–30 months, 30–36 months, 36–42 months, and 42–48 months time periods postsurgery). The number of outpatient clinic visits for the 6 months preceding surgery was collected. A dry ear was defined as a well-epithelialized mastoid cavity with the absence of drainage, moisture, mucous, or granulation tissue that remained stable for two or more clinic visits. The main outcomes of interest were achievement of a dry ear, time to development of a dry ear, and mean number of outpatient clinic visits per 6-month period. Medical records were reviewed to extract demographic information, including characteristics of ear disease, tobacco use, history of previous surgical interventions, history of tympanostomy tube placement, surgical technique and observations, and the number of outpatient clinic visits. We compare outcomes between obliterated versus nonobliterated mastoid bowls, as well as the impact of primary versus secondary obliteration. We review our experience of surgical outcomes of canal-wall-down mastoidectomy with and without obliteration for the management of chronic ear disease, with particular attention to the establishment of a dry, low-maintenance ear, and the frequency of outpatient clinic follow-up. The need for frequent clinic follow-up has been reported for canal-wall-down mastoidectomy ( 3, 5), and is a significant source of frustration and resource burden to individuals and the health system. A reduction of mastoid recess depth and overall volume may also eliminate areas of chronic moisture ( 2, 8), theoretically reducing the frequency of needed cleaning. Obliteration reduces the volume of the mastoid cavity ( 2, 9), thereby reducing the meatal size needed for effective clinic management. Mastoid obliteration has been proposed to facilitate healing and epithelialization ( 8, 9), and can be performed at the original canal-wall-down procedure or in a delayed secondary procedure after the canal wall is taken down ( 9). Obliteration can be performed using a variety of techniques or materials, including but not limited to autologous bone chips and dust ( 10), hydoroxyapetite ( 11, 12), cartilage ( 13), and periosteal-pericranial flaps ( 8). Mastoid obliteration has gained increasing attention as an adjunct to open mastoid procedures ( 2, 9). These concerns have led some to primarily advocate for the use of canal-wall-up mastoidectomies ( 4), or propose the reconstruction of the ear canal-mastoid partition ( 6) or obliteration of the mastoid cavity ( 2, 7- 9). Open mastoid procedures have been criticized for the unfavorable cosmetic appearance of a large meatoplasty, the perpetual need for intermittent cleaning, as well as the propensity for chronic moisture and intermittent super-infection or drainage ( 2, 5).
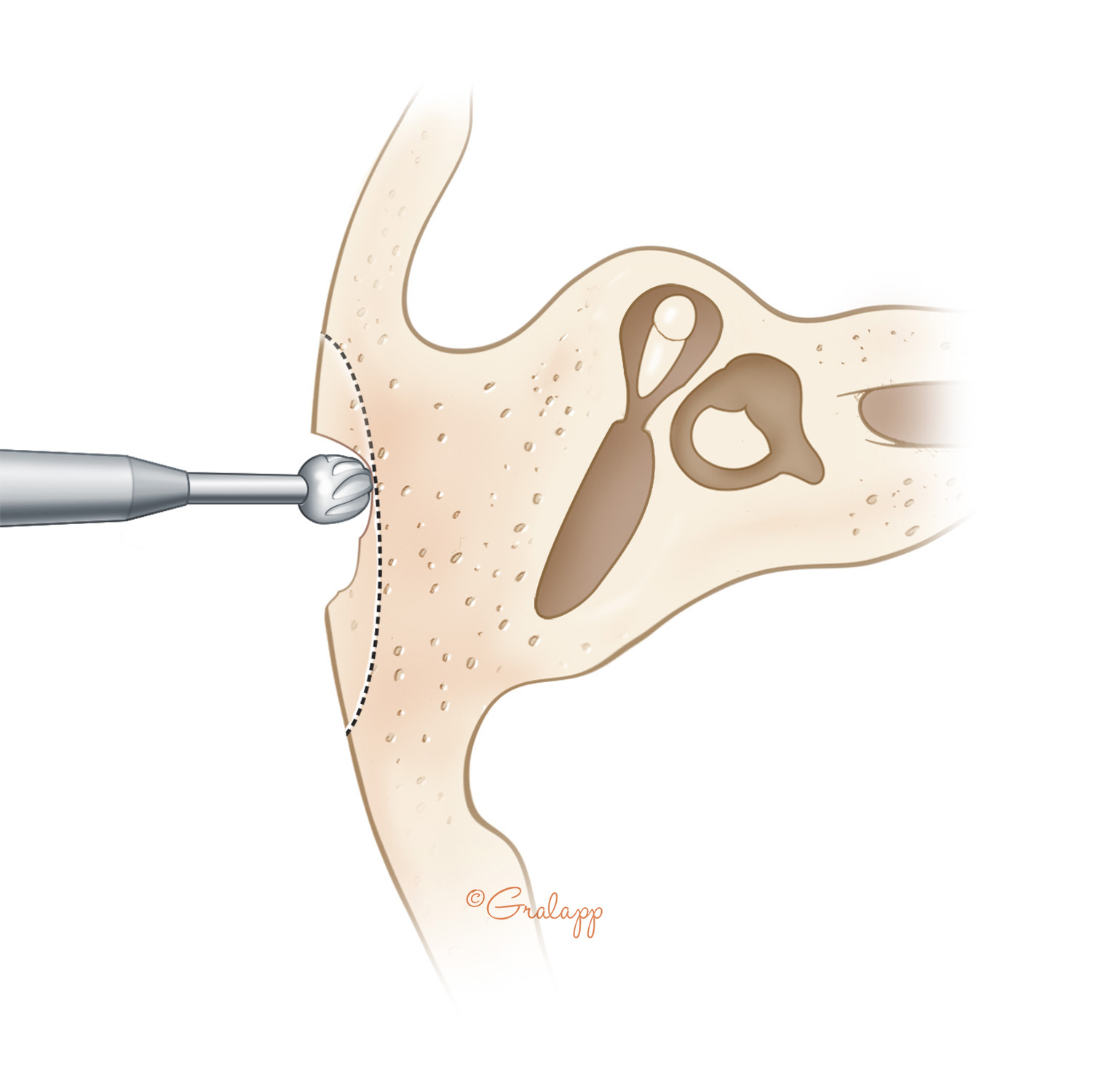
Despite careful observation of best practices including mastoid saucerization, removal of the mastoid tip, lowering of the facial ridge, and creation of an adequately sized meatus ( 4), moisture may persist in areas of the mastoid bowl leading to stasis of mucoid exudates, localized areas of infection, and underlying mucosal changes. Persistent moisture, infection, and drainage is problematic in as many as one-third of patients requiring revision surgery following canal-wall-down mastoidectomy ( 3), which may be attributed to mucosalized surfaces, persistent cell tracts, or poorly ventilated areas opening into the mastoid bowl ( 2). Exteriorization of attic and mastoid disease with a canal-wall-down mastoidectomy has a high rate of success in achieving a safe ear ( 1), but there is a need for continuous care including a high incidence of moisture resulting in drainage or crusting ( 3). The primary goal of surgical intervention for chronic ear disease is the development of a safe, dry, and low-maintenance ear ( 1, 2).

